What is Tongue-tie?Embryological remnant of tissue in the midline between the undersurface of the tongue and the floor of the mouth that restricts normal tongue movement. Definition of the International Affiliation of Tongue-tie Professionals
Describing Tongue-tieMany words are used to describe tongue-tie, such as "mild", "little", "slight", "posterior" "anterior", "partial" and a long list of others. However, because it presents in many different forms, these descriptors are inadequate to determine how each presentation will affect you and your baby. In order to assess if the tongue movement is affected, a thorough examination of function, together with a feeding history and visual feeding assessment is NECESSARY.
|
|
What does a tongue need to do?A normal tongue should be able to:
1. Extend beyond the lower gum with the tip thin, rounded and flat 2. The tip (without notching or changing shape) should be able to lift to at least the centre of the mouth cavity (1cm or more from the lower gumline) 3.The tongue should be round, thinnish and flat and be able to create a central groove to cup the nipple. (sometimes described as "cupping") This should extend to towards the throat. 4.The tongue should be able to move freely around the mouth, from side to side and each side should be able to move and lift freely while staying in shape. (no bunching) 5. The tongue should be allowed to move freely around the mouth and elevate enough to clean milk from its surface on the hard palate. 6. The tongue needs to cup the breast and hold it against the palate to maintain a vacuum during the suck/swallow breathe cycle. |
What might a baby with tongue-tie do?1. Tip might come to gum line but it may:
- come to a blunt point - form a central notch of the tongue as it stretches, (pulling on a restriction on the underside of the tongue) - curl under as it stretches toward the gum line 2. The tongue may not be able to lift at all or it may distort, bunch or form some notching as it attempts to move. An elevation of <1cm may be a problem. A whitish line may become visible as the blood flow is pinched from the frenum while it tries to stretch. 3. The tongue may have times when it appears thin and round but sometimes looks "boxy". As the moves back in the mouth it may notch in the centre. Sometimes the outer part of the tongue may flip out leaving the central tongue area 'humped". This is sometimes described as a "stringray" tongue. 4. The tongue may bunch or turn, only from the restriction under the tongue and may not maintain a thin rounded shape. 5. The back of the tongue may not elevate enough to clean the milk on the palate, leaving a constant white patch at the back of the tongue which may be mistaken for thrush. |
How is it treated?The extra tissue (frenum) is revised using either scissors or laser. This sounds simple but actually there are many variations on this treatment. At PREMIER HEALTH we use round tip scissors and revise the frenum to the base of the tongue, ensuring that full movement is restored in line with the restriction found during the examination.
Not all those who treat tongue-tie use this method, some will revise just the film of tissue (may not restore full range of movement), some will use clamps on the frenum before the procedure or a dentist may use a laser. At Premier Health we go through a thorough consent process after consultation so you can make an informed choice about the procedure. We will also be there to support you through the feeding immediately after and help address other feeding concerns. In some cases, the lip frenulum may be a problem as well, this may also need to be revised. |
|
Why are there differing opinions about tongue-tie?Many health professionals want to avoid intervention unless there a clear benefit to be gained from the procedure. Longstanding, robust evidence exists about the effect on breastfeeding, bottle-feeding (many babies have trouble with a bottle as well) and long-term oral health.
This evidence supports early and thorough revision of tongue and lip frenums to prevent a cascade of ongoing, predictable consequences. Research from the UK suggests that if feeding has not improved after 24-48hrs of lactation support, the frenum should be revised. Recent studies support this, showing that leaving a longer time only prolongs and exacerbates the problems for mother and baby. Support for breastfeeding in Australia is very poor and many families are struggling with a baby who is have some difficulty feeding and advice that will not contribute to succeeding at breastfeeding. Please see our Country Report to see the extent of how bad it is for families in Australia. |
Please click on the picture for our FRENOTOMY AFTERCARE INSTRUCTIONS
|
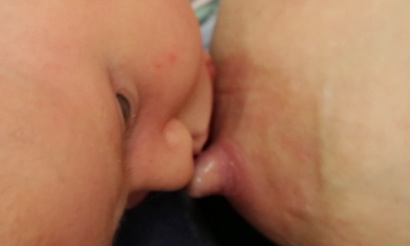
Signs you might noticeA creased or damaged nipple may look OK from the outside but is a sign that the nipple is in the wrong place. Many mothers are told it looks OK despite these obvious symptoms.
Poor attachment - shallow - dimpling at the sides of mouth while feeding - Sore nipples - not always but may be grazed or creased - Baby coming off and on breast - can't maintain suction - Dribbling during feeding (this may happen with a bottle as well) - Windy baby - swallows a lot of air - Noisy or long feeds (not a lot of swallowing, bottle feeding babies may have similar issues) - May have very strong suction - Partially white tongue - lots of sucking but little swallowing, has to stop after a swallow to catch a breath |
Why the confusion?Babies are born with strong instincts, they know what they need to do and they do it. Mothers have hormonal support in the first 4-6 weeks to allow breastfeeding to become established.
Initially a baby will swallow what is released, but as he grows and cannot feed effectively enough to empty your breasts he may grow frustrated. Maintaining breastfeeding relies on your baby to remove the milk you have available so, as the support hormones reduce (4-6wks), behaviour and feeding may also change. This is confusing because mothers are usually doing all the right things. The affect on you and your baby will be individual, as your breasts, milk release and baby's mouth are all unique. Not all women will have nipple trauma or problems with growth and not all baby's with TT will have an obvious heart-shaped tongue. When we reviewed our clients over a 24 month period we found that SHALLOW GAPE and POOR MILK TRANSFER were the most consistent signs of poor tongue function. |